Managing an Eye Which Cannot Close Properly
Case Study: The GP and optometrist have important roles
Dr Charles Su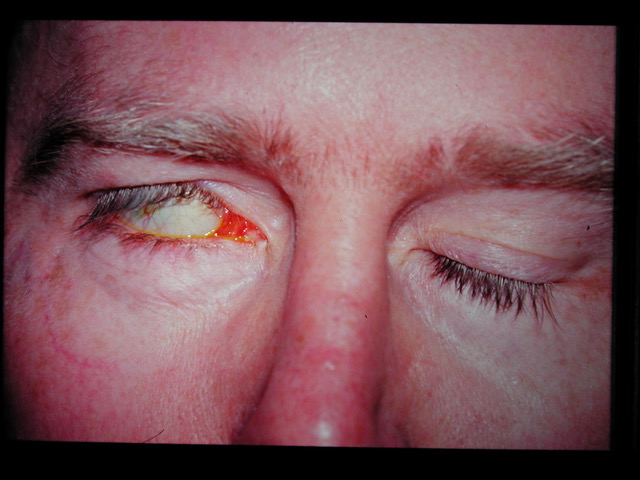
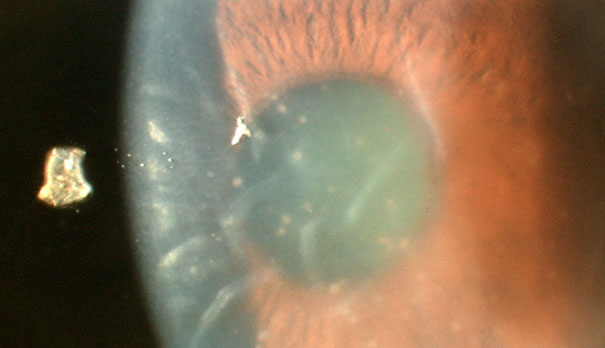
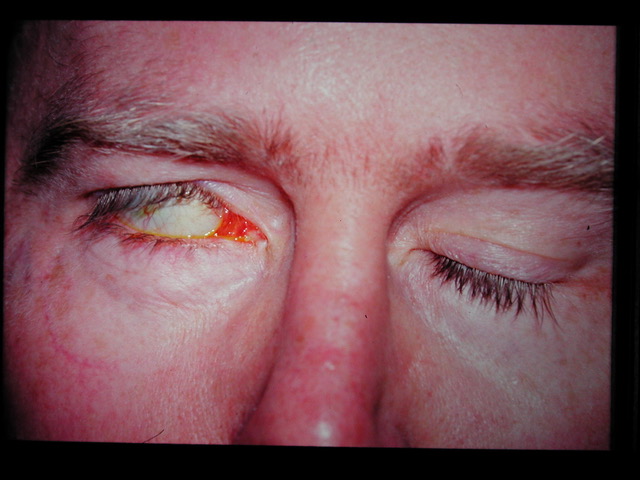
This picture is of a patient with a facial paresis. He is unable to close the right eye completely.
Of course, establishing a diagnosis and ensuring that causes such as intracranial pathology and neural infiltration with SCC is paramount, and neuro-imaging can be necessary.
Preventing damage to the ocular surface is also important.
Here are a few tips:
1. Make sure that there is no loss of corneal sensation.
2. Regular artificial drops EVEN WHEN THERE IS NO DISCOMFORT.
3. Warn the patient that the ointment is messy …
and will block good vision for a few minutes, but use a thick oily ointment before bed, not just a gel. Poly Visc and Refresh Night Time ( Lacri Lube) are examples of ointments which should be liberally put into the lower lid fornix.
4. A Moisture Chamber can reduce night time drying.
A large piece of clear cling wrap such as Glad Wrap, folded up into the size of a credit card, can be taped loosely over the eye region on the affected side with ordinary or paper tape, after placement of the ointment, before sleep, so that the passage of air over the partially open eyelids is reduced through the night. This is more effective than wearing a fabric eye patch with an elastic band, which can slip, and which is less impermeable.